Every phlebotomist has heard and maybe even witnessed patients' "war stories" of bad experiences with venipuncture. Major patient’s complaints include:
- being stuck too many times
- enduring the discomfort while the person drawing the blood digs or fished around for a vein
- experiencing excruciating pain
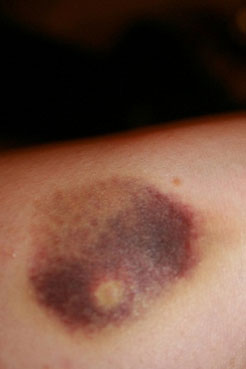
- experiencing extensive bruising
As a phlebotomist you can remedy these situations by doing the following:
- Put the patient at ease by reassuring and getting them to relax.
- Patients who are unpleasant, uncooperative, or abusive often exhibit this behavior as a defense mechanism for their anxiety about the puncture. Remain calm, professional and pleasant with all patients.
- Meticulous confirmation of patient identification, especially in emergency situations is important to prevent drawing the wrong patient.
- Always have the patient's arm resting firmly on a solid surface, either the drawing station or a rolled support. This prevents the patient from pulling back from the needle with the initial puncture.
- Properly anchor the vein by pulling the skin taunt with the thumb to prevent the vein from rolling. CLSI recommends only using the thumb to anchor, and not the "C" anchor, where the vein is straddled between the thumb and index finger. However, this position may be needed on elderly patients with veins that move or roll, especially those in the hand. But be aware that if the patient pulls away in this position, the needle could recoil as it comes out of the patient's vein, springing back into the index finger.
- Unless you need the patient to make a fist to locate the vein, don't have the patient make a fist. Making a fist tightens the muscles of the arm and makes the needle puncture more painful. This is especially true on heavily muscled arms.
- Rotate the patient's wrist to confirm whether a tendon is present. You will feel definite movement with a tendon, but not a vein.
- It is permissible and especially considerate for patients with fragile or loose skin and hairy arms to tie the tourniquet over lightweight clothing such as shirts and blouses. The pinching of the skin by the tourniquet is often more painful to the patient than the actual venipuncture.
- When you fail to get any or enough blood, be very careful what you say to the patient. Comments such as, "Your vein must have blown" are particularly frightening to the patient. Do not attempt more than two punctures.
- Everyone has a bad day or gets flustered by a particular patient. Be aware when this happens and take a break. Make it a practice among the phlebotomy team to give each other "grace" times.
- Keep the angle of the needle entry at 15 degrees or less. The more parallel the needle is to the vein, the easier it is to access. This is one of the advantages of using the short, butterfly needle.
- Because of the high number of nerves in the hand and the thin skin, hand sticks are very painful. Use a 23 gauge butterfly needle.
- Before any redirecting of a needle, it is important to ascertain where the needle is in relation to the missed vein by gently palpating the tip of the needle. Then pull out the needle to where the bevel is just below the skin surface. Turn the tip of the needle into the new direction, and gently move the needle forward until the vein is encountered.
- Know the length of your needle and be able to visualize it, so you always know how much is in the patient. It is very rare that a vein will be deeper than one half the length of a 1 inch needle.
- On inpatients, it is especially important to coordinate with the nursing staff and check with the log board the number of draws that a patient has done that day.
- Several pokes for tests that could have been ordered together are no joke.

